Key Takeaways
-
Chronic wounds significantly affect both physical health and emotional well-being, often leading to anxiety, depression, and reduced quality of life.
-
Advancements in wound care—from growth factors to amniotic membrane products—can accelerate healing and reduce psychological distress.
-
A holistic approach that includes mental health support, lifestyle changes, and innovative treatments leads to better outcomes for patients.
Chronic wounds are more than just a physical condition; they deeply impact a person’s mental health, well-being, and quality of life. For patients and medical professionals alike, understanding the connection between physical healing and psychological support is critical to improving outcomes.
This post will explore how chronic wounds affect mental and emotional health, the science of wound healing, and the latest advancements in wound care that can accelerate the healing process. Whether you’re a medical professional or someone living with a chronic wound, this guide will provide insights to help you or your patients heal faster—both physically and mentally.
Understanding Chronic Wounds
Chronic wounds are wounds that fail to heal within 4 to 12 weeks, even with medical intervention. They are often a result of underlying health conditions such as diabetes, venous insufficiency, or weakened immunity.
One common example is venous leg ulcers, which are open wounds on the lower leg caused by poor circulation. For many people, such wounds can become a recurring issue, leading to long-term suffering, discomfort, and frustration.
Treatment for chronic wounds typically involves addressing the root causes, caring for the wound itself, managing pain, and supporting mental health. Because the nature of chronic wounds often requires long-term care, their impact extends far beyond physical symptoms, often taking a significant toll on emotional well-being.
When wounds fail to heal, patients may feel trapped in a cycle of ongoing appointments, costly treatments, and declining self-esteem. This can lead to withdrawal from social situations and difficulty managing daily responsibilities. That’s why addressing chronic wounds comprehensively is crucial—not just to close the wound, but to help patients regain their quality of life.
The Healing Process
Wound healing is a complex and highly coordinated biological response. It involves the regeneration of tissue, the control of infection, and the regulation of inflammation. These stages don’t always happen in a clean sequence—in fact, they often overlap.
When the body’s natural healing cycle is disrupted, it can halt progress and lead to chronic conditions. Recognizing the importance of each phase helps clinicians and caregivers understand when intervention is necessary.
Inflammation
The inflammatory phase is the body’s first response to injury. Proinflammatory cytokines and white blood cells flood the area to fight infection and clear debris. These essential molecules set the stage for new tissue growth.
This stage is crucial for preventing complications and setting a strong foundation for recovery. If inflammation lingers or becomes excessive, it can stall healing and lead to further tissue damage.
Proliferation
During this phase, fibroblasts and epithelial cells work hard to repair the damaged tissue. They produce collagen and other proteins, laying the groundwork for new skin to form.
As new tissue forms, capillaries develop to supply oxygen and nutrients, supporting healthy regeneration. This is often where visible progress occurs, but it remains a delicate process that must be closely monitored.
Remodeling
Finally, the remodeling phase strengthens and reorganizes the newly formed tissue. This is the longest phase and can extend for months after the initial injury.
Proper wound care during this stage ensures the final tissue is strong and functional. Skipping or rushing this phase can lead to fragile scars or wound recurrence.
Wound Care and Treatment Options
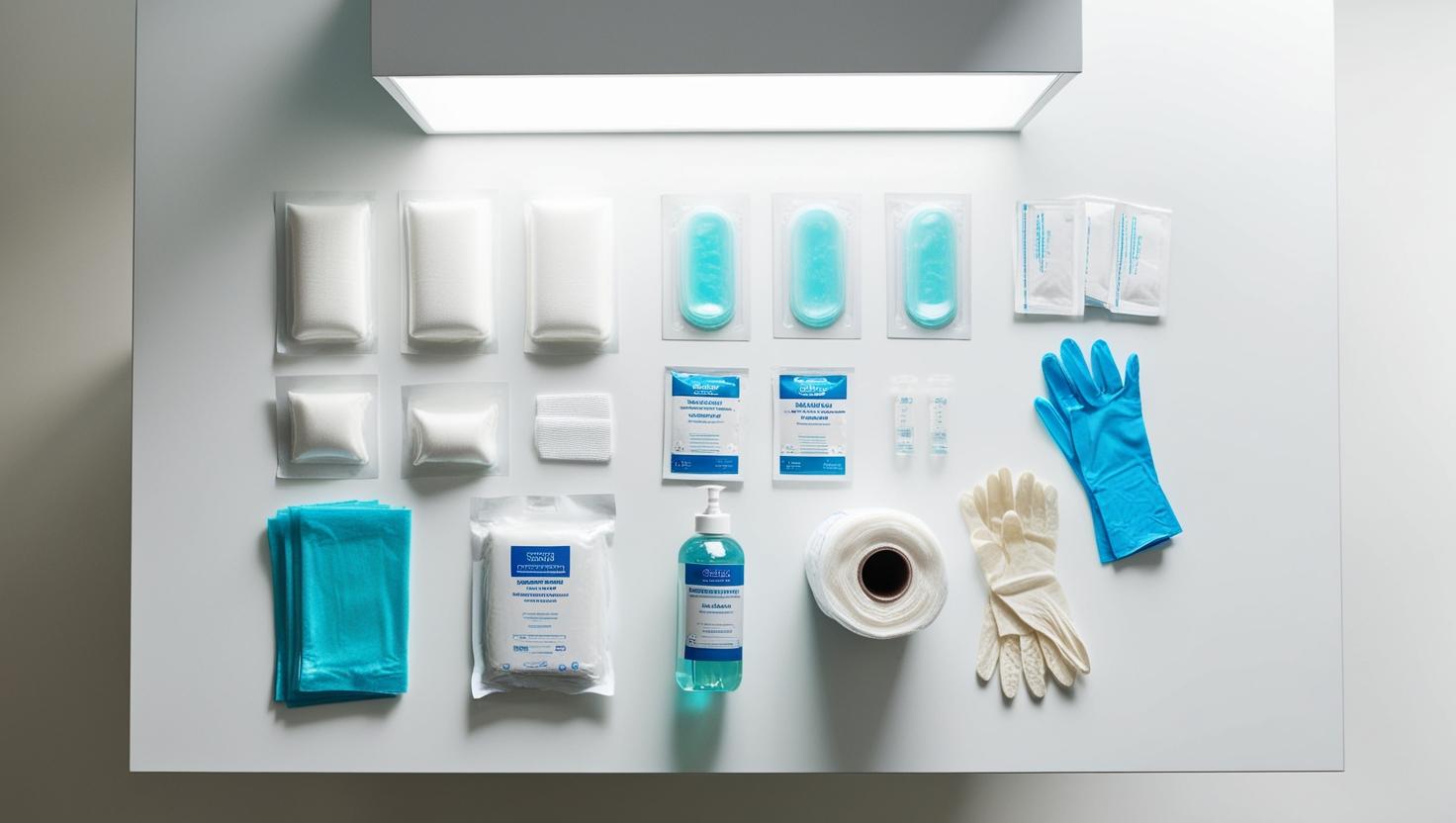
Treating chronic wounds requires more than just cleaning and dressing the affected area. A personalized and consistent approach makes all the difference in the healing timeline and the patient’s comfort.
Selecting the right products and techniques can significantly improve healing outcomes, reduce complications, and restore mobility and confidence. Below are some of the most common options used by wound care professionals.
Moist Wound Dressings
Keeping wounds moist, rather than dry, accelerates healing. There are many types, including hydrogels, foam dressings, and hydrocolloids. Each serves a specific purpose depending on the wound type.
These dressings help maintain the perfect environment for cell regeneration while reducing pain and the risk of infection. The key is to match the dressing type with the wound’s stage and moisture level.
Dressings That Prevent Infection
Some dressings—like antimicrobial gauze—help protect the wound from harmful bacteria while soaking up excess fluid. Changing the dressing regularly is critical to avoid leaks or loss of efficacy.
Infection is one of the leading causes of delayed healing. Antimicrobial dressings are a proactive way to mitigate this risk, especially in patients with compromised immune systems.
Growth Factors
Growth factors can be applied directly to the wound to stimulate cell growth and accelerate healing.
They serve as biochemical signals that tell cells how to act, making them especially helpful in chronic wounds that have become stalled in a particular phase. Many of these treatments are now readily available and easy to integrate into clinical care plans.
Pro Tip: Consult with your supplier or wound care specialist to explore regenerative products that enhance growth factor activity.
Advanced Treatment Options
In some cases, conventional wound care just isn’t enough. When healing stalls despite best efforts, advanced modalities can offer new hope and faster outcomes.
These treatments may require specialized equipment or procedures, but they can dramatically improve healing rates in patients with hard-to-treat wounds.
Amniotic Membrane Wraps
Amniotic membrane wraps are an innovative and highly effective option in modern wound care. Derived from the innermost layer of the placenta, these biological dressings contain natural growth factors, anti-inflammatory proteins, and antimicrobial properties that promote faster and more complete healing.
These wraps provide a protective barrier while supporting cellular regeneration, reducing scar tissue formation, and minimizing pain. They’re especially beneficial for non-healing wounds, diabetic ulcers, pressure sores, and post-surgical sites.
Because amniotic membranes are immune-privileged, they carry a low risk of rejection and can be safely used across a wide range of patients. Many wound care specialists now consider them a preferred option when standard treatments fall short.
If you’re a provider looking to integrate cutting-edge biological therapies into your wound care strategy, amniotic membrane wraps are a smart, science-backed solution worth exploring.
Hyperbaric Oxygen Therapy (HBOT)
By having patients breathe in pure oxygen under high pressure, HBOT floods the bloodstream with oxygen, promoting faster healing. Research has shown its effectiveness in treating chronic wounds, especially diabetic foot ulcers.
The added oxygen boosts the body’s immune response and helps tissues repair more efficiently. HBOT sessions are often used in combination with other therapies for maximum benefit.
Skin Grafts
For large wounds that won’t close naturally, skin grafts are an effective option. Grafts use the patient’s own skin (or donor tissue) to cover and promote repair over the affected area.
This approach is particularly helpful when there’s extensive tissue loss. Grafts act as scaffolds, encouraging native cells to rebuild the skin over time.
Pain Management and Mental Health
Pain and emotional distress often go hand in hand, especially when healing feels slow or uncertain. Managing both is essential not only for comfort but also for long-term recovery success.
Patients living with chronic wounds frequently report a diminished quality of life, increased isolation, and even clinical depression. A multidisciplinary approach can help mitigate these effects.
Managing Pain
-
Use dressings designed to be less adhesive and cause minimal discomfort when changed.
-
Clean the wound with a gentle saline rinse.
-
Rely on over-the-counter medications like ibuprofen or acetaminophen for mild to moderate pain.
In more severe cases, physicians may prescribe stronger pain relief or consider adjunct therapies like nerve blocks or topical anesthetics.
Supporting Mental Health
The emotional weight of living with a chronic wound can be overwhelming. Patients experience anxiety, feelings of hopelessness, and depression—but psychological support can make a significant difference. Counseling, support groups, and mindfulness practices help individuals cope with these challenges.
Building a strong support network—both professional and personal—can help patients regain a sense of control over their condition.
Healthcare providers should routinely screen for depression and anxiety in wound care patients and offer referrals for mental health services when needed.
Nutrition and Lifestyle Changes for Faster Healing
Healing is not just about bandages and treatments—it’s also about making the body stronger from within. Nutrition and lifestyle play vital roles in the body’s ability to recover and regenerate tissue.
By adopting healthier habits, patients not only improve wound outcomes but also enhance their overall wellness and energy levels.
Protein-Packed Diet
Foods rich in protein, like eggs, fish, and lean meats, provide the building blocks for tissue repair.
Adequate protein intake supports cell regeneration, immune function, and collagen synthesis—all critical to wound healing.
Hydration
Drinking sufficient water ensures nutrients circulate effectively and reach the wound.
Dehydration slows healing and increases the risk of complications. Encouraging regular fluid intake is an easy yet powerful step toward recovery.
Quit Smoking
Smoking impairs blood flow, directly slowing down the healing process. Reducing stress and avoiding harmful habits are just as vital for recovery.
Even cutting back can make a difference. Smoking cessation programs are often available through healthcare providers and community health centers.
Overcoming Barriers to Healing
Even with the best care, wounds can hit roadblocks. Identifying and addressing these barriers early can prevent complications and keep healing on track.
Personalized care plans, early intervention, and patient education are essential for overcoming these obstacles.
Infections
Bacterial infection is a common problem. Wound cultures and antibiotics are essential tools to fight infections and reestablish healthy healing conditions.
Signs of infection include redness, odor, swelling, and increased pain. Timely intervention can prevent more serious complications like cellulitis or sepsis.
Venous Insufficiency
When poor blood flow prevents healing, compression therapy and certain surgical interventions can make a difference.
Patients with underlying vascular conditions may benefit from referrals to specialists who can provide long-term solutions.
Emerging Trends in Wound Healing
The future of wound care is here—and it’s rapidly evolving. Cutting-edge innovations are transforming how we treat chronic wounds, making healing faster, more effective, and more accessible.
These technologies not only improve patient outcomes but also reduce the overall cost of care by shortening healing times and preventing complications.
Nanotechnology
Nanoparticles can be used to deliver treatments directly to the wound site, improving outcomes.
These particles can carry antibiotics, growth factors, or anti-inflammatory agents exactly where they’re needed, enhancing effectiveness while minimizing side effects.
Biomaterials
Advanced materials help mimic human tissue and enable faster recovery.
These synthetic or bioengineered dressings interact with the body to stimulate cell growth and manage moisture levels more precisely than traditional dressings.
Collaboration in Care
Partnerships between researchers, healthcare providers, and specialists in wound healing products pave the way for new discoveries and better treatment options.
This team-based approach ensures patients receive the most up-to-date and effective treatments available.
A Holistic Approach to Healing

Chronic wounds are more than a physical condition—they’re a challenge that impacts daily life and mental health. Faster healing doesn’t just mean relief from physical pain; it offers patients a chance to reclaim their independence, confidence, and happiness.
When providers integrate advanced wound care with emotional support and lifestyle changes, the result is a truly holistic model that empowers patients to thrive—not just survive.
At Advanced Wound Products, we understand the burden chronic wounds place on both patients and providers. That’s why we offer a full line of amniotic membrane products and regenerative solutions tailored for wound care specialists seeking better, faster outcomes.
If you’re looking to elevate your wound care program, contact Advanced Wound Products today to learn more about our advanced healing technologies and clinical support services.
Together, let’s accelerate healing and transform lives.



